Open heart coronary surgery

Everything you need to know about coronary open heart surgery (CABGs)!
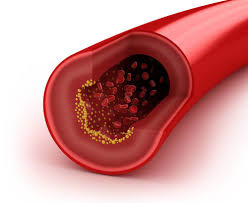
Every year, a large number of patients undergo open heart surgery for coronary artery bypass surgery to treat coronary artery blockage and its complications. Although this procedure is life-saving, it still has its own tips and risks that people with coronary artery disease should be familiar with.
The system of veins, or the black veins of the legs, is a dual system. In this way, both the deep veins and superficial veins known as “saphenous veins” can direct the blood in the legs to the heart through the saphenous veins. For this reason, the superficial veins of the leg can be removed easily and no problems will be caused in the venous blood flow of the leg. This vein, which has a length of 50 to 60 cm, is easily removed, and first the valves of the pigeon’s nest and its branches are separated and divided into several parts according to the length of the transplanted veins.
During coronary artery bypass surgery, one side of these black veins is sewn to the main artery of the body, i.e. the aorta, and the other side is sewn to the coronary arteries of the heart after the stenosis, and in this way, the blocked and narrow coronary area is bypassed. Blood flow is re-established in the post-coronary stenosis area. Usually, 2 to 4 of these grafts are used in each bypass operation.
Venous grafts have a thinner wall than the coronary arteries of the heart and the rest of the arteries, and their diameter is greater than the diameter of the coronary arteries, that’s why the tolerance of these grafts against arterial pressure is low and there is a possibility of their blockage over time. Venous grafts usually last about 5 to 10 years, after which up to 50% of these types of grafts will narrow and become blocked again. After 10 to 15 years, only 15% of these links are open, but considering that the re-blocking of these links happens gradually and over the years, the heart muscles can tolerate the re-blocking better and therefore suffer less. Chest pain.
Venous grafts can be easily treated with stents and angioplasty in case of obstruction and re-stenosis, and require less open heart surgery. Although all the venous connections are blocked and the risk of re-operation of the heart is not high, re-operation can be done. Open heart re-operation is associated with more risks than the first operation and is associated with a lack of veins due to their use in the first operation.

Due to the limitations of the use of black veins for coronary artery grafting, the use of arteries for cardiac artery grafting has received much attention. The justification for this interest in using arteries is that the walls of arteries are thicker and they can withstand intravascular pressure more than veins. Also, the diameter of the used arteries is almost similar to heart vessels and they create better and more regular blood flow. LIMA artery
In the past years, arteries such as the “radial artery of the hand” and “visceral arteries of the abdomen” have been used for this purpose, but the best results have been seen with the use of the “Internal Mammary Artery”. This artery inside the chest wall on the right and left side of the chest is separated from the “subclavian or subclavian” artery and moves downward and supplies blood to the space between the ribs. This artery has a lifespan of more than 20 years and can provide safe and secure blood supply to the heart for a long time.
Due to the importance of the internal chest artery LIMA, most surgeons prefer to transplant this vein to the most important coronary artery of the heart which is the left descending artery of the heart or “LAD” and use leg vein grafts for other veins.
Artificial veins
Artificial veins are tubes made of “Teflon” or “Nylon” that are produced in different dimensions and diameters and can be used to connect all kinds of veins inside the body. In the past years, the use of these artificial veins in the heart has not had good results, and the speed of blockage and blood clot formation in them has been higher than that of venous and arterial grafts. Therefore, today this type of transplant is not used for heart bypass surgery and their use is limited to people whose natural vessels, whether veins or arteries, cannot be used for heart surgery


But unfortunately, in general, some of the weight of about 30% of patients returns as a result of lack of exercise and improper diet.
6. Can I eat again like before?
Yes, after the first few months you can eat normal foods (but your portions will be smaller) and your obesity-related medical problems will improve, as will your energy and overall health.
7. Will everyone notice my bariatric surgery?
Most weight loss occurs in the first 6 to 12 months after surgery, so people may notice a change in your appearance, but it’s your choice whether or not to share your decision about bariatric surgery.
Telling your friends, acquaintances, colleagues and others is your decision, but we recommend that you definitely have some supporters in this way; Because bariatric surgery and weight loss are difficult. Having a supportive friend or family member on your weight loss journey can be helpful.
8. Will I have sagging skin after losing weight?
Most patients do not experience skin sagging after bariatric surgery. But some people may want to do cosmetic procedures to treat sagging skin! Several factors that can affect sagging skin; Age, genetics and hydration. Additionally, it is recommended that you begin exercising approximately 6 weeks after surgery to prevent skin sagging and build lean muscle.
Types of treatment methods for sagging skin after severe weight loss:
Sport
Cosmetic surgeries such as abdominoplasty and panniculectomy
laser therapy
Use of collagen creams
9. Can I get pregnant after bariatric surgery?
Yes, you can still get pregnant after bariatric surgery, and some patients actually find it easier to get pregnant after losing the weight they gain from bariatric surgery. We recommend that you wait at least 18 to 24 months after surgery before trying to get pregnant. It is important to tell your OB/GYN that you have had bariatric surgery and to stay in touch with your surgeon to ensure a safe pregnancy.